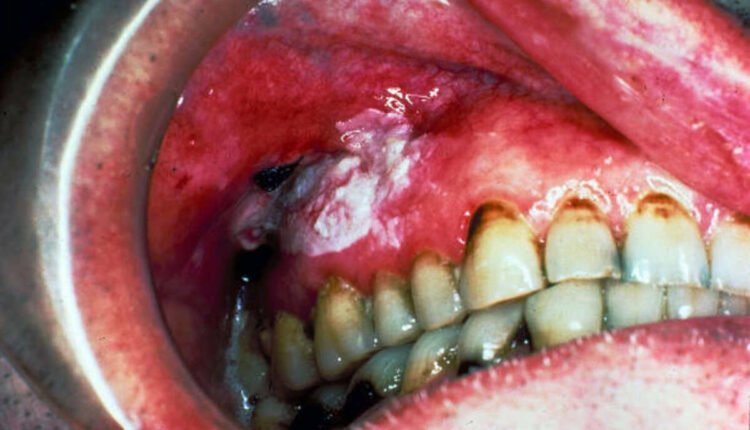
Leukoplakia is a type of oral cancer, and the most common symptoms are white patches in the mouth. It generally affects men between the ages of 50 and 70. Only about one percent of cases affect people younger than 30. These patches are not painful, but if they occur in large enough numbers or with red spots, they should be evaluated by a doctor.
Nonhomogeneous leukoplakia
There are several different types of nonhomogeneous leukoplakia lesions. While the majority of these lesions are benign, some are not. Nonhomogeneous leukoplakias may be nodular, irregularly flat, or erythematous. Verrucous leukoplakia, for example, is an aggressive type of leukoplakia that may progress to cancer.
Nonhomogeneous leukoplakia can be diagnosed by histopathology. The histological analysis allows the clinician to exclude other lesions and assess the degree of epithelial dysplasia. Because nonhomogeneous leukoplakia is associated with an increased risk of malignant transformation, it is critical to have a biopsy performed to rule out other causes of this lesion.
Nonhomogeneous leukoplakia is a condition in which the oral tissue is primarily white or blends white and red and often takes on an irregular shape. The most common treatment for this lesion is surgery. Surgical resection is the most effective method for removing pathologic tissue, allowing for examining margins and pathology. In addition, surgical resection is less invasive, and there are fewer risks of scarring. Using CO2 laser excision techniques has several advantages over a scalpel, such as reducing intraoperative bleeding and decreasing the need for flaps.
Oral hairy leukoplakia
Oral hairy leukoplakia (OHL) is a rare and asymptomatic inflammatory lesion on the tongue that develops in immunocompromised patients. It is characterized by a non-removable white patch on the lateral border of the tongue. It was first described as pathognomonic for HIV infection but is now recognized as a benign immune response. It is associated with Epstein-Barr virus (EBV), but not all cases are positive Epstein-Barr virus (EBV). It may result from another condition, but it is often asymptomatic and does not require therapy.
Oral hairy leukoplakia is non-tender plaques that develop on the lateral border of the tongue. They may appear and disappear spontaneously and may cause mild pain or dysesthesia. They can also change the sensation of taste and temperature. If left untreated, this condition can lead to AIDS and must be treated as soon as possible.
Treatment for oral hairy leukoplakia is a variety. A health professional can often diagnose the condition through a physical examination. If a virus causes it, the healthcare provider may prescribe antiviral medications. Otherwise, the infection may require treatment with antifungal medications. In some cases, a healthcare provider may suggest that you undergo a biopsy of a single sore to confirm the diagnosis. However, this is only necessary if the patches are abnormal. It may also be done if cancer or rare conditions are suspected.
Causes
Leukoplakia is a common oral condition most often caused by tobacco use (smoking and smokeless tobacco). According to the Mayo Clinic, three out of four tobacco users will develop the condition. It may also develop on the lips, tongue, and cheeks in people who have damaged or jagged teeth or wear dentures that don’t fit correctly.
Although there is no known cure for leukoplakia, it can be prevented. Symptoms include white patches on the inner surface of the mouth. If left untreated, the lesions can progress to squamous cell carcinoma, a slow-growing type of oral cancer.
As with other cancers, leukoplakia can be caused by several factors. Heavy alcohol consumption and smoking increase the risk of leukoplakia. Heavy drinkers are eight times more likely to develop the condition than non-drinkers.
Treatment
Fortunately, leukoplakia is highly treatable with proper diagnosis and treatment. This condition is typically asymptomatic, although it may lead to oral squamous cell carcinoma. Treatment options will vary, depending on the type of cells present. A biopsy may be required to determine if leukoplakia is cancerous or not.
A biopsy can be done through incisional or excisional methods. An incisional biopsy requires the removal of the leukoplakia patch and provides a definitive diagnosis. It may be performed using a scalpel, laser, or cryoprobe. Sometimes, patients need a course of medicine to suppress the symptoms and prevent further growth.
Non-surgical treatment for leukoplakia is usually the preferred option for most patients, but it isn’t without risk. The cumulative malignant transformation rate of leukoplakia is 11.6% over ten years without surgical resection. Furthermore, lesions with higher degrees of epithelial dysplasia are more likely to progress to cancer. Therefore, the most effective oral leukoplakia treatment helps you keep the irritation to a minimum.